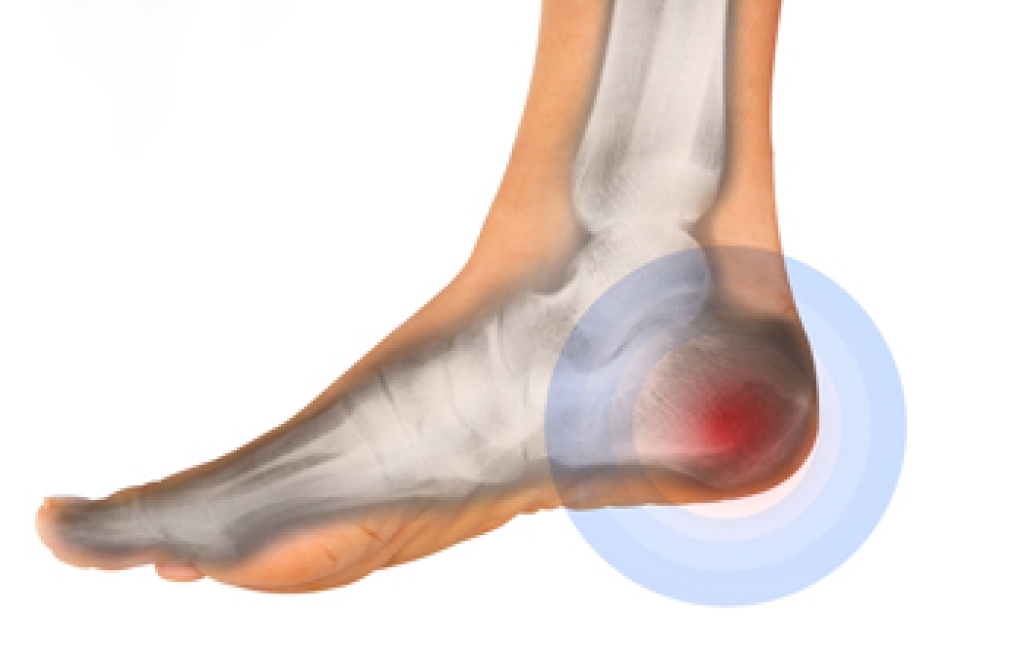
Ankylosing spondylitis is a long-term form of arthritis that causes inflammation in the body. It often affects the spine, but it can also involve the feet. This condition includes inflammation where tendons attach to bone and can lead to heel pain. The plantar fascia, a thick band of tissue on the bottom of the foot, may become irritated and cause discomfort while walking. The Achilles tendon at the back of the heel can also become inflamed, leading to stiffness and swelling. Some people notice pain after rest or during the first steps of the day. Such ongoing inflammation may affect foot movement and balance. A podiatrist can evaluate foot pain and order imaging to confirm the diagnosis. Treatment options include custom orthotics, bracing, and targeted treatment to reduce strain. If you have foot problems as a result of ankylosing spondylitis, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and appropriate treatment.
When dealing with systemic disease of the feet, it is extremely important to check the affected areas routinely so that any additional problems are caught quickly. If you have any concerns about your feet and ankles contact Robert Dunne, DPM from Lake Washington Foot and Ankle Center. Our doctor will assist you with all of your podiatric needs.
Systemic Diseases of the Feet
Systemic diseases affect the whole body, and symptoms usually are displayed in the feet. This condition can make a patient’s ability to walk unbearable. Systemic diseases include gout, diabetes mellitus, neurological disorders, and arthritis.
Gout – is caused by an excess of uric acid in the body. Common symptoms include pain, inflammation, and redness at the metatarsal/phalangeal joint of the base big toe. Gout can be treated by NSAIDs to relieve pain and inflammation, and other drugs that lower the acid levels in the body.
Diabetes mellitus – is an increase in the level of blood sugar that the body cannot counteract with its own insulin. Failure to produce enough insulin is a factor in Diabetes.
Diabetes of the Feet
Diabetic Neuropathy – may lead to damaged nerves and affect the feet through numbness and loss of sensation.
Peripheral Vascular Disease – can restrict the blood flow to the feet, and often times lead to amputation of the feet.
If you have any questions please contact our offices located in Melbourne and Palm Bay, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.